Cheat Sheet to Effective Burnout Strategies for HCPs

What Treatment Strategies Work Best for Healthcare Professionals with Burnout? [2025 Cheat Sheet]
What treatment strategies work best for healthcare professionals with burnout? The strongest results come from combining individual interventions (mindfulness, therapy, boundaries) with organization-level changes (smaller caseloads, better scheduling, real leadership support). Research is clear: organization-directed strategies drive bigger, more durable gains than individual efforts alone—but the best outcomes happen when both are in play.
Quick Answer: Top Treatment Strategies That Actually Work
| Individual Strategies | Organizational Strategies |
|---|---|
| Mindfulness-based stress reduction | Workload reduction and schedule changes |
| Cognitive Behavioral Therapy (CBT) | Reducing administrative burdens |
| Setting firm work-life boundaries | Improving staffing ratios |
| Peer support groups | Leadership training and support |
| Physical activity and sleep hygiene | Flexible work schedules |
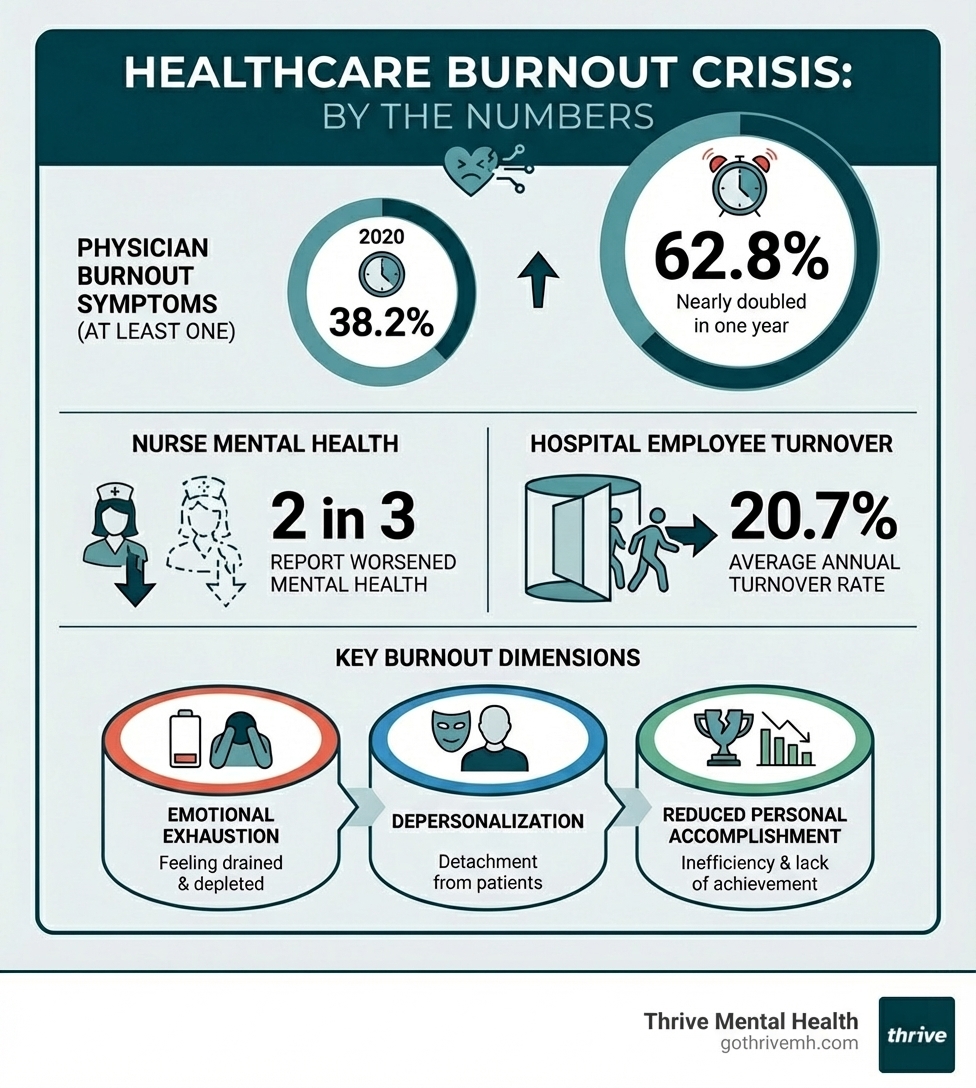
Burnout isn’t just feeling wiped after a long shift. It is a state of emotional exhaustion, depersonalization (feeling detached or numb with patients), and a reduced sense of accomplishment caused by chronic workplace stress that never lets up.
And it’s everywhere in healthcare right now.
- 63% of physicians report at least one symptom of burnout.
- Two in three nurses say their mental health has worsened over the past year.
- Nearly half of all healthcare professionals who leave the profession cite burnout as the reason.
This is not about personal weakness. It is about a system that is burning out the people holding it together.
This cheat sheet cuts through the noise. You will see what treatment strategies work best for healthcare professionals with burnout, backed by research and grounded in real-world practice. You will learn:
- What you can do this week to lower your burnout symptoms
- Which system-level fixes actually move the needle
- How to tell when weekly therapy is not enough—and what to do next
Whether you are a physician in Miami, a nurse in Tampa, or a therapist in Orlando, you will walk away with a clear roadmap to reclaim your well-being without walking away from your career.
I’m Nate Raine, CEO of Thrive Mental Health. For over a decade I have worked where mental health, healthcare operations, and digital care models intersect. At Thrive, we deliver evidence-based Intensive Outpatient (IOP) and Partial Hospitalization (PHP) programs—including fully virtual IOP—for adults and young professionals across Florida. I have seen again and again how intensive, flexible programs custom for professionals can change the trajectory when simple self-care and once-a-week therapy are not enough.
Let’s walk through what actually works.
Quick what treatment strategies work best for healthcare professionals with burnout? definitions:
For a deeper dive into higher levels of care, see our overview of Intensive Outpatient (IOP) and PHP programs.
The Alarming Reality: Why Healthcare Professionals Are Burning Out
Burnout in healthcare is no longer just a buzzword; it’s a full-blown crisis, driven by systemic failures rather than individual shortcomings. We see our dedicated healthcare professionals pushed to their limits by an unrelenting combination of factors that erode their well-being and, ultimately, compromise patient care. The statistics paint a grim picture: a staggering 62.8% of physicians reported at least one burnout symptom in 2021, a sharp increase from 38.2% in 2020. For nurses, the situation is equally dire, with two in three reporting their mental health has worsened over the past year.
The primary culprits:
- Excessive Workload: The sheer volume of patients, coupled with staffing shortages (average turnover rate: 20.7%), means healthcare professionals are constantly doing more with less.
- Administrative Burdens: Mountains of paperwork, complex billing procedures, and regulatory compliance eat into valuable patient-facing time. 43% of healthcare administrators experience moderate to high burnout.
- EHR Frustration: Electronic Health Records systems are often clunky and non-intuitive, adding to documentation burden rather than easing it.
- Lack of Autonomy: Healthcare environments can be highly hierarchical, limiting input into decision-making. Research suggests lack of control contributes to 23% of physician burnout.
- Poor Work-Life Balance: Demanding schedules and shift work disrupt personal lives. Over half of U.S. nurses are considering leaving their jobs within six months.
- Emotional Toll: Constant exposure to suffering and critical illnesses leads to compassion fatigue and moral injury.
- Staff Shortages: Persistent lack of adequate personnel exacerbates all other factors.

How does physician burnout specifically impact patient care quality and safety?
The consequences of physician burnout extend far beyond the individual, directly threatening patient care:
- Increased Medical Errors: Burnout correlates with increased medical errors. Emergency physicians with burnout scores above 35 (Maslach Burnout Inventory) show significantly prolonged patient wait times.
- Reduced Patient Satisfaction: Depersonalization leads to diminished patient satisfaction and decreased treatment compliance.
- Depersonalized Care: Emotional detachment means patients feel like numbers rather than individuals.
- Longer Wait Times: Exhausted physicians work slower and make more mistakes requiring rework.
- Decreased Compliance: Patients are less likely to follow medical advice without empathetic connection.
- System-Wide Consequences: Burnout contributes to declining healthcare quality, reduced productivity, and significant economic costs. With 20.7% turnover rates and half of nurses considering leaving, the exodus of experienced professionals creates a toxic cycle.
Individual vs. Systemic Fixes: What Actually Moves the Needle?
When people ask, “What treatment strategies work best for healthcare professionals with burnout?”, the default answer is often: do more self-care. Meditate. Sleep more. Be more resilient.
Those help—but they are not enough.
Research consistently shows that organization-directed interventions deliver larger, more durable reductions in burnout than physician-directed or individual-only interventions. Personal resilience matters, but it cannot fully offset chronic understaffing, unsafe workloads, or toxic culture.
The reality:
- Individual strategies help you survive the next shift.
- Systemic strategies change the conditions that are burning you out in the first place.
- The best outcomes combine both.

Here’s how individual and organizational interventions stack up—and how they work together:
| Individual-Focused Interventions | Organization-Directed Interventions |
|---|---|
| Mindfulness & Meditation: Brief mindfulness interventions can improve well-being, reducing stress and anxiety. | Workload Reduction: Rescheduling hourly shifts, reducing patient load, and ensuring adequate staffing. |
| Therapy (CBT, DBT): Cognitive Behavioral Therapy helps reframe negative thought patterns, while Dialectical Behavior Therapy builds emotional regulation skills. | Structural Changes: Streamlining workflows, optimizing EHR systems, and reducing administrative burdens. |
| Exercise & Sleep Hygiene: Regular physical activity and sufficient rest are fundamental to physical and mental health. | Flexible Scheduling: Offering more control over schedules and providing adequate paid time off. |
| Communication Skills Training: Improves interpersonal interactions and reduces conflict, improving job satisfaction. | Leadership Training & Support: Developing empathetic, supportive leaders who prioritize staff well-being. |
| Peer Support Groups: Fosters a sense of community and reduces feelings of isolation. | Fair Rewards & Recognition: Implementing recognition programs and ensuring equitable compensation. |
| Self-Reflection & Values Alignment: Reconnecting with personal purpose and ensuring it aligns with institutional values. | Promoting Justice & Fairness: Ensuring transparency in decision-making and fair treatment for all staff. |
Key takeaway: Burnout is primarily an organizational problem with individual consequences. The most effective treatment strategies for healthcare professionals with burnout:
- Pair personal tools (like CBT, mindfulness, and boundaries) with
- Concrete organizational changes (like staffing fixes, schedule control, and leadership accountability).
If you are already doing all the self-care and still feel stuck, it does not mean you are failing. It likely means the problem is bigger than any one person—and that it may be time to consider higher-support options like IOP or PHP that give you intensive therapy while you advocate for systemic change.
For a practical, personal game plan, keep reading: the next section is your Burnout Recovery Toolkit.
Your Personal Burnout Recovery Toolkit [Actionable Steps]
You cannot fix a broken system alone—but you can take back control of what is in your hands right now. These strategies do not replace organizational change, but they can lower your symptoms, protect your mental health, and buy you breathing room while bigger fixes catch up.
What are the most effective individual strategies for healthcare professionals to manage and mitigate burnout symptoms?
-
Mindfulness and Meditation
Even brief mindfulness interventions can reduce stress and improve emotional regulation. Start with 5-10 minutes daily:- Guided audio on your commute
- Box breathing between patients
- Body scan before bed
-
Setting Firm Boundaries
- Say no to extra shifts when at capacity
- Stop checking EHR and email during off-hours
- Protect one weekly block of non-work time
-
Protecting Personal Time
- Schedule hobbies and family time as real appointments
- Treat personal time cancellations as seriously as clinic add-ons
-
Physical Activity
- 10-20 minutes of walking or stretching on workdays
- Longer sessions on off days doing something enjoyable
-
Sleep Hygiene
- Consistent sleep-wake schedule when possible
- Dark, cool, quiet room; limit screens 30-60 minutes before bed
- Avoid heavy caffeine late in the day
-
Peer Support Groups
- Join or start a peer support huddle on your unit
- Use structured groups with clear confidentiality
-
Seeking Professional Therapy
- CBT helps change burnout-fueling thoughts
- DBT builds emotion regulation and boundary-setting skills
- Consider IOP or PHP if weekly therapy isn’t enough
Thrive Mental Health offers specialized IOP and PHP programs for healthcare workers across Florida with evening virtual options.
-
Communication Skills Training
- Learn boundary-setting without burning bridges
- Practice clear communication to reduce friction
-
E-Mental Health Interventions
- Secure therapy platforms
- Skills-based apps for CBT and mindfulness
- Online therapy options
-
Reconnecting with Personal Values
- Ask: Why did I go into healthcare?
- Find small ways weekly to practice those values
-
Improving Work-Life Integration
- Coordinate schedules with family
- Use commute rituals to separate work from home
- If hours are unsustainable, that’s data—not failure
If you’re reading this from a call room in Orlando, a clinic in Miami, or a hospital in Jacksonville thinking “I’m way past self-care,” you might be right. That’s when providers at Thrive step into virtual or hybrid IOP/PHP for concentrated support. Learn more in our guide to CBT for professionals.
What Treatment Strategies Work Best for Healthcare Professionals with Burnout? [An Organizational Playbook]
If you are in leadership asking “What treatment strategies work best for healthcare professionals with burnout?”, here is the hard truth:
- Yoga classes without staffing fixes will not save your team
- Resilience workshops without schedule control can make burnout worse
Healthcare organizations must shift from blame to support and treat burnout as an occupational hazard demanding structural solutions:
- Reduce exhaustion drivers
- Increase control, fairness, and recognition
- Make mental health support routine, confidential, and stigma-free
This work directly affects patient safety, turnover costs, and revenue from Miami to Jacksonville and across the state of Florida.
How can healthcare organizations effectively measure burnout and track interventions?
You cannot fix what you do not measure. Start with clear, repeatable measurement:
-
Standardized Tools
- Maslach Burnout Inventory (MBI): Gold-standard measuring emotional exhaustion, depersonalization, personal accomplishment
- Copenhagen Burnout Inventory (CBI): Assesses personal fatigue, work exhaustion, client strain
- Single-Item Burnout Scales: Quick, high-frequency check-ins
-
Regular Staff Surveys
Run confidential surveys twice yearly tracking:- Workload and staffing safety
- Perceived leadership support
- Psychological safety
-
Tracking Turnover
With 20.7% average hospital turnover:- Monitor turnover, vacancy time, transfer patterns
- Flag high-risk areas (ED, ICU, oncology, primary care)
-
Patient Safety Metrics
Burnout shows in:- Medical error rates
- Patient satisfaction scores
- Door-to-doc times, LOS, readmissions
-
AMA Organizational Biopsy
The AMA Organizational Biopsy evaluates system burnout drivers.
How can the stigma around seeking mental health support be reduced?
Stigma keeps clinicians sick and silent. Make getting help safe and expected:
-
Leadership Vulnerability
Leaders openly acknowledging stress sends the message: Getting help is part of being a safe clinician -
Normalizing Conversations
Make well-being a standing agenda item in meetings, grand rounds, orientations -
Confidential Access
- Clinicians access therapy confidentially
- Service use does not jeopardize licensure or promotion
- Clear written policies backing this up
- Offer virtual IOP programs for staff in Jacksonville, Miami, Tampa, and Orlando
-
Peer Support Programs
Structured peer support after adverse events or chronic stress -
Destigmatizing Language
Frame burnout as predictable response to stressors, not character flaw -
Integrating Wellness
- Protect breaks in real schedules
- Recognize units improving well-being metrics
- Partner with providers like Thrive for IOP/PHP tracks covered by Cigna, Optum, Florida Blue
When organizations pair cultural shifts with concrete workload changes, burnout drops, retention improves, patient outcomes follow. See Thrive’s Intensive Outpatient programs for staff support strategies.
Finding the Right Help: Programs & Resources That Actually Move the Needle
Wellness apps and one-off workshops can be a nice start—but for many burned-out healthcare professionals, they barely scratch the surface. When symptoms are severe or long-standing, you need evidence-based therapy and, often, a higher level of care than a weekly 50-minute session.
Here is what works best, and when.
-
Evidence-Based Therapeutic Approaches
-
Cognitive Behavioral Therapy (CBT):
Helps you identify and challenge the thoughts and beliefs that keep you trapped in burnout cycles—like perfectionism, catastrophizing, and all-or-nothing thinking. CBT is one of the most studied and effective treatments for stress, anxiety, and depression in healthcare workers. Learn more in our guides to CBT for professionals and CBT for stress management. -
Dialectical Behavior Therapy (DBT):
Originally developed for intense emotional dysregulation, DBT is powerful for clinicians who:- Feel constantly on edge or emotionally flooded
- Struggle to set and hold boundaries
- Swing between detachment at work and overwhelm at home
DBT builds four core skills: mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness.
-
Mindfulness-Based Stress Reduction (MBSR):
Structured mindfulness programs like MBSR can reduce stress, improve focus, and increase self-compassion—key buffers against burnout. Brief mindfulness interventions have already shown effectiveness in improving provider well-being.
-
-
When Weekly Therapy Is Not Enough: IOP and PHP
If you are still asking yourself “What treatment strategies work best for healthcare professionals with burnout when I already tried therapy?”, the answer is often: step up the level of care.
-
Intensive Outpatient Programs (IOP):
- Several hours of group and individual therapy per week
- Multiple days per week, often with evening options
- You live at home and may be able to keep modified work hours
-
Partial Hospitalization Programs (PHP):
- More intensive than IOP (often daytime, most weekdays)
- Best for severe burnout with significant depression, anxiety, or functional impairment
- You return home at night instead of staying inpatient
Thrive Mental Health specializes in virtual and in-person IOP and PHP for adults and young professionals in Florida, including:
- Virtual IOP for maximum flexibility
- PHP programs when you need more structure
Our programs are insurance-friendly—we work with major plans such as Cigna, Optum, and Florida Blue (coverage varies by plan). You can verify coverage in minutes using our Start benefits check tool.
-
-
Promising Programs & Resources
Alongside dedicated treatment, these resources can support both individuals and organizations:
-
AMA STEPS Forward® Program:
Practical modules and toolkits focused on practice efficiency, workflow redesign, and physician well-being. -
Mindful Practice® Workshops:
Programs (often run through academic centers like the University of Rochester) that build mindfulness, reflection, and communication skills for clinicians. -
The Happy MD Training:
Coaching and training custom to physicians focused on stress reduction, boundaries, and practice redesign. -
Mayo Clinic’s Physician Well-Being Resources:
Research-backed strategies and toolkits for both individual physicians and healthcare systems. -
Stanford Medicine WellMD Center:
A leader in physician well-being research and system-level interventions. -
Downloadable Toolkits:
Practical guides like the “Free Anti-Burnout Toolkit for Healthcare” (from Bucketlist Rewards) can help HR and leadership teams build reward and recognition structures that support engagement.
-
For a deeper dive into how higher levels of care fit into a burnout recovery plan, you can explore our broader psychotherapy services and related educational content on the Thrive blog.
Frequently Asked Questions About HCP Burnout Treatment
What is the first step to treating healthcare burnout?
The first step is to name what is happening: chronic fatigue, cynicism, irritability, emotional numbing, or feeling like nothing you do matters. Recognize that burnout is a systemic, work-related condition, not a personal flaw. From there, take one tangible next step:
- Talk to a trusted peer or supervisor
- Schedule a confidential therapy consult
- Use your organization’s EAP or wellness resources
If symptoms are intense or getting worse, consider an evaluation for a higher level of care such as IOP or PHP.
Can you fully recover from burnout?
Yes. Many clinicians do recover—but recovery usually requires both personal and systemic change. On the personal side, that might include therapy (CBT or DBT), boundaries, and time away from unsafe workloads. On the system side, it often involves role changes, better staffing, schedule adjustments, or transferring to a healthier environment. The more your workplace addresses the root causes—workload, control, fairness, and support—the more durable your recovery will be.
What level of care is best for severe burnout?
For severe burnout that overlaps with major depression, anxiety, or serious functional impairment, once-a-week therapy is often not enough. Intensive Outpatient (IOP) or Partial Hospitalization (PHP) programs provide:
- Multi-hour therapy sessions
- Several days per week
- Structured groups plus individual support
These levels of care are designed for people who need more support than weekly therapy but do not need inpatient hospitalization. Thrive offers virtual and in-person options across Florida.
Do insurance plans like Cigna, Optum, or Florida Blue cover IOP/PHP for burnout?
Coverage varies by plan, but many commercial insurers in Florida—including Cigna, Optum, and Florida Blue—do cover IOP and PHP when symptoms meet medical necessity criteria (for example, significant functional impairment, risk factors, or co-occurring depression/anxiety). The fastest way to know is to use our 2-minute Start benefits check tool or call us to verify benefits.
How do I know if I need virtual IOP vs. in-person treatment?
Virtual IOP is often a good fit if you:
- Have a stable home environment
- Prefer privacy and flexibility (especially around busy shifts)
- Live far from a treatment center (for example, in smaller cities around Tampa Bay, the Panhandle, or South Florida)
In-person care can be better if you:
- Need more structure and separation from home
- Prefer or require face-to-face interaction
At Thrive, we offer both virtual IOP and hybrid models so you and your clinician can choose what fits best.
Your Path to Recovery Starts Now
Burnout is a predictable response to a broken system, not a verdict on your strength, competence, or compassion. But if you ignore it, the costs climb fast:
- Your health suffers.
- Your relationships strain.
- Your clinical judgment and patient care can be impacted.
The most effective answer to what treatment strategies work best for healthcare professionals with burnout is a dual approach:
- Individual care: CBT, DBT, mindfulness, boundaries, and—when needed—stepping up to IOP or PHP instead of trying to white-knuckle through another year.
- Organizational change: Safer staffing, schedule control, lower admin burden, and leaders who treat burnout as a safety issue, not a character flaw.
At Thrive Mental Health, we build programs specifically for professionals in demanding fields—including physicians, nurses, therapists, and allied health workers—in Florida. We combine:
- Evidence-based treatment (CBT, DBT-informed skills, MBSR)
- Flexible virtual and in-person IOP/PHP options, including evenings
- Insurance-friendly access, working with major plans like Cigna, Optum, and Florida Blue where available
If you are in Tampa Bay, Miami, Orlando, Jacksonville—or anywhere in Florida—you do not have to choose between your career and your mental health.
Summary: The best treatment strategies for healthcare professionals with burnout blend personal tools with system-level fixes and, when needed, higher levels of care like IOP/PHP. You do not have to wait until everything collapses to get that level of support.
Ready for support? Thrive offers virtual and hybrid IOP/PHP programs with evening options. Verify your insurance in 2 minutes (no obligation) → Start benefits check or call 561-203-6085. If you’re in crisis, call/text 988.
Reviewed by Anna Green, LMHC, LPC, Chief Clinical Officer at Thrive Mental Health. Anna is licensed in Florida (MH23391), Indiana, South Carolina, North Carolina, and Arizona, and was named to Women We Admire's Top 50 Women Chief Clinical Officers of 2025.
This article is for informational purposes only and is not a substitute for individualized clinical advice or specific insurance verification.